Vive La (Antibiotic) Résistance? Learn more about this year’s Antibiotic Awareness Week! By Our Student Pharmacist, Cass Baker.
If you’ve ever been prescribed an antibiotic, you probably remember that your doctor or pharmacist told you to finish the entire 5-10 day treatment prescribed. “Why is that so important?”, you might ask. Finishing all of your medication might seem like a small detail, but it is actually a strategy to prevent a growing issue worldwide called antibiotic resistance.
What is antibiotic resistance?
Antibiotics are an essential tool to combat bacterial infections in humans and animals. However, every time bacteria are exposed to an antibiotic, they can develop mechanisms to combat the way the antibiotic is designed to kill them. Over time, this natural process can render commonly prescribed antibiotics ineffective.
How exactly does antibiotic resistance work?
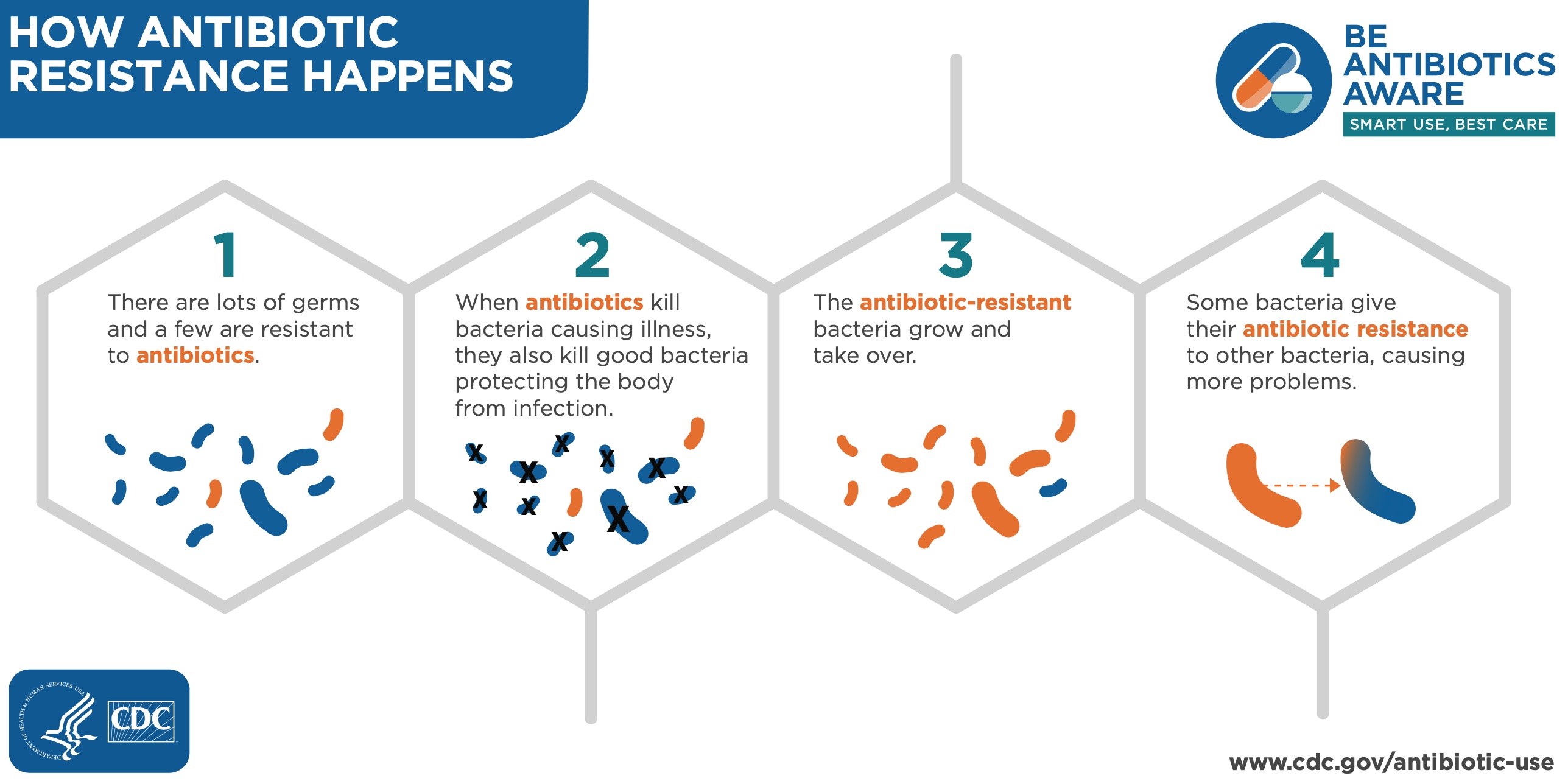
Bacteria typically form colonies as they infect the human body, but not all of the individual cells are killed by the antibiotic prescribed at the same time. Some individual colonies may be killed after one day, while other colonies are stronger and require more time to be exposed to the antibiotic before they are killed. If the resistant bacteria survive, as shown in the below diagram as orange bacteria in steps 1 and 2, they can grow to form new colonies that are harder to treat.
Okay, but if antibiotic resistance happens naturally, then what’s the concern?
Unfortunately, an increasing number of antibiotic-resistant infections such as pneumonia, strep throat, gonorrhea, and foodborne bacterial infections occur in the U.S. The Centers for Disease Control and Prevention (CDC) estimate that 2.8 million antibiotic-resistant infections occur in the U.S. every year, causing infections that are not readily treatable and 35,000 deaths per year. Infections that are becoming resistant to commonly used antibiotics drive up healthcare costs, because they typically require longer and more expensive treatments. Sometimes they even cause extended hospital stays, potentially exposing patients to hospital-specific infections, as well.
The spread of resistant infections threatens all countries worldwide, regardless of economic status. Additionally, there are fewer research prospects for new antibiotics than in the past, which means that resistant infections are more difficult than ever to treat, if not impossible. Fortunately, there are simple behaviors that both patients and prescribers should practice in order to control the spread of these infections.
What should I do to help prevent or control antibiotic resistance?
Because antibiotics remain essential to treat and prevent certain infections, they absolutely should be used when the benefits of treatment outweigh the risks of resistance or side effects. Therefore, it is crucial to avoid antibiotic overuse when it is not necessary. Antibiotics are only effective for treating bacterial infections. Patients should refrain from demanding an antibiotic when a prescriber diagnoses them with a viral infection such as the flu; and prescribers should refrain from prescribing antibiotics unless they diagnose or suspect a bacterial infection. These practices ensure that the antibiotics we use today will continue to be effective for as long as possible.
Another important behavior that patients should implement is taking a prescribed antibiotic exactly how it was written, for the number of days that it was prescribed. For example, if you are prescribed enough tablets to last five days, be sure to take all five days’ worth! Many patients will start to feel better after taking antibiotics for a couple of days and stop treatment prematurely. However, this increases your risk of more resistant bacteria surviving the shorter than intended antibiotic treatment, and the original infection re-growing stronger than before.
Finally, it is important to remember to protect yourself and others from the spread of infections as well to reduce the number of yearly antibiotic-resistant cases. Believe it or not, practicing basic hygiene such as washing your hands and preventative measures such as vaccinations, cooking food thoroughly, and safe sex practices decreases your chances of being prescribed antibiotics in the future, reducing the burden of developing new antibiotics on the healthcare industry.
Be sure to check out the World Health Organization’s (WHO) website for World Antimicrobial Awareness Week (which occurs this year from November 18-24) for more information on antibiotic resistance initiatives from across the globe!
Resources: